Diarrhea is a bowel movement (defecation) by the number of stools more than normal (normal 100-200 cc / hr feces). With the stool is liquid / solid half, may be accompanied by an increased frequency.
According to WHO (1980), diarrhea is watery bowel movements more than 3 times a day.
Diarrhea is divided into two based on the onset and duration, namely acute and chronic diarrhea (Mansjoer, A.1999, 501).
Etiology of Diarrhea
1. Infection factor: bacteria (Shigella, Shalmonella, Vibrio cholera), virus (enterovirus), parasites (worms), Candida (Candida Albicans).
2. Parenteral factors: infections of other parts of the body (OMA often occurs in children).
3. Malabsorption factors: Carbohydrates, fats, proteins.
4. Dietary factors: Food stale, poisonous, too much fat, cooked vegetables underdone.
5. Psychological factors: Fear, anxiety.
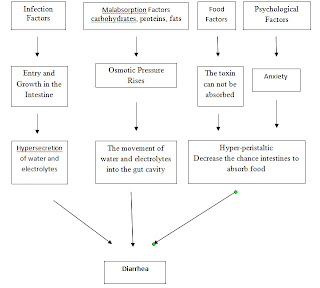
Pathophysiology Diarrhea
Nursing Assessment Nursing Care Plan for Children with Diarrhea
1. Identity
Noteworthy is the age. Episodes of diarrhea occurred in the first 2 years of life. The incidence is highest age group 6-11 months. Most intestinal bacteria stimulate the immune response to infection, it helps explain the decreased incidence of disease in older children. At the age of 2 years or more active immunity begins to form. Most cases are due to asymptomatic intestinal infection and enteric bacteria spread mainly clients are not aware of the infection. Economic status are also influential, especially from diet and treatment.
2. Main complaint
Defecate more than 3 times
3. Disease History Now
Defecation: greenish yellow color, mixed with mucus and blood or mucus only. Watery consistency, frequency of more than 3 times, spending time: 3-5 days (acute diarrhea), more than 7 days (persistent diarrhea), more than 14 days (chronic diarrhea).
4. In the past history of disease
Previous history of diarrhea, use of antibiotics or corticosteroids long term (changes in Candida albicans from saprophyte to parasites), food allergy, respiratory infection, UTI, OMA, measles.
5. History of Nutrition
In children ages toddler foods given as in adults, the share of a given 3 times per day with additional fruit and milk. Malnutrition in children toddler age are particularly vulnerable. Good food management, food hygiene and sanitation, hand washing habits.
6. Family Health History
There was one family who had diarrhea.
7. Environmental Health History
Food storage at room temperature, lack of hygiene, neighborhood.
Nursing Diagnosis and Nursing Interventions for Children with Diarrhea
1. Fluid And Electrolyte Imbalances related to fluid loss secondary to diarrhea.
Objectives: after nursing action for 3 x 24 hours, fluid and electrolyte balance is maintained to the fullest.
Expected outcomes:
- Vital signs are within normal limits
- Turgor elastic, mucous membranes moist lips, the eyes do not cowong, the crown is not concave.
- Consistency of bowel movements soft, frequency 1 time per day
Interventions and Rational :
1) Monitor signs and symptoms of fluid and electrolyte
R / decrease the volume of fluid circulation causing mucosal dryness and urinary concentration. Early detection allows immediate fluid replacement therapy to correct the deficit
2) Monitor intake and output
R / Dehydration can increase the glomerular filtration rate was adequate to make the output to remove the waste.
3) Measure weight every day
R / Detecting loss of fluid, decrease of 1 kg of body weight equal to 1 liter of fluid loss
4) Encourage the family to drink lots of 2-3 liters / day
R / Replacing the lost fluids and electrolytes orally
2. Imbalanced Nutrition Less Than Body Requirements related to diarrhea or excessive output and intake of less.
Objectives: after the action at home on hospital care for nutritional needs are met
Expected Outcomes:
- Increased appetite
- Increased body weight, or normal according to age
Interventions and Rational:
1) Discuss and explain about the restriction diet (high fiber foods, fatty foods and water is too hot or cold)
R / high fiber, fat, water is too hot / cold can stimulate irritate the stomach and intestinal tract.
2) Create a clean environment, away from the smell that odor or waste, serve food in warm
R / situation a comfortable, relaxed will stimulate the appetite.
3) Give the patient time to rest - sleep and reduce the excessive activity
R / Reduce excessive energy consumption
4) Monitor intake and output in 24 hours
R / Knowing the amount of output can plan the amount of food
3. Risk for Imbalanced Body Temperature related to the process of infection secondary to diarrhea.
Objectives: After making maintenance actions performed for 3 x 24 hours, there was no increase in body temperature
Expected outcomes:
- Body temperature within normal limits (36 to 37.5 C)
- There is no sign of infection (rubur, dolor, color, tumors, fungtio leasa)
Interventions and Rational:
1) Monitor the body temperature every 2 hours
R / Early detection of abnormal changes in body function (an infection)
2) Give a warm compress
R / stimulates the central thermostat to lower the body's heat production
3) Collaboration of antipirektik
R / Stimulate the central thermostat in the brain.
4. Risk for impaired skin integrity related to increased frequency of diarrhea.
Objectives: after nursing actions while in hospital, skin integrity is not compromised
Expected outcomes:
- No irritation: redness, abrasions, cleanliness maintained
- Families are able demonstrate perianal care properly
Interventions and Rational:
1) Discuss and explain the importance of maintaining a bed
R / hygiene prevents germs breeding
2) Demonstrate and involve the family in caring for perianal (if wet clothing and replace the bottom and base)
R / Prevent the occurrence of skin irritation is not expected, because of humidity and acidity of the stool
3) Adjust bed or seated position with an interval of 2-3 hours
R / Smooth vascularization, reducing the emphasis of the old so that does not happen ischemia and irritation.
5. Risk for impaired growth and development related to body weight decreased continuously.
loading...
nursing home east sussex
ReplyDeleteThe Doctor shall describe and have individual describe in words the relationship of diabetic issues and eating plan, and the individual shall give a return description is his / her own words. (this breastfeeding mediation will help clear up and misconseptions and strengthen the medical value of a healthy type two diabetic issues person diet
whenever a child has an diarrhea, we should take them into doctor. free cna training
ReplyDeleteThis provides a lot of great information for parents! I have three children of my own, and when my youngest had a lot of intestinal issues I found myself learning a lot of these care instructions. If the problem persists, you should always opt for a critical care test to ensure it's not a symptom of a more serious underlying condition. The test is non-invasive and gives you results very quickly, so it's perfect for little ones who are obviously not thrilled to be in the hospital or doctor's office in the first place.
ReplyDelete